The “Goldilocks Effect”
Author: Dr. Stephen Chaney
How much carbohydrates should we eat?
 The low-carb wars rage on. Low-carb enthusiasts claim that low-carb diets are healthy. Many health experts warn about the dangers of low-carb diets. Several studies have reported that low-carb diets increase risk of mortality (shorten lifespan).
The low-carb wars rage on. Low-carb enthusiasts claim that low-carb diets are healthy. Many health experts warn about the dangers of low-carb diets. Several studies have reported that low-carb diets increase risk of mortality (shorten lifespan).
However, two recent studies have come to the opposite conclusion. Those studies reported that high carbohydrate intake increased mortality, and low carbohydrate intake was associated with the lowest mortality.
One of those studies, called the Prospective Urban Rural Epidemiology (PURE) study was published just last year. It included data from 135,335 participants from 18 countries across 5 continents. That’s a very large study, and normally we expect very large studies to be accurate. The results from the PURE study had low-carb enthusiasts doing a victory lap and claiming it was time to rewrite nutritional guidelines to favor low-carb diets.
Whenever controversies like this arise, reputable scientists are motivated to take another look at the question. They understand that all studies have their weaknesses and biases. So, they look at previous studies very carefully and try to design a study that eliminates the weaknesses and biases of those studies. Their goal is to design a stronger study that reconciles the differences between the previous studies.
 Such a study has just been published (SB Seidelmann et al, The Lancet, doi.org/10.1016/S2468-2667(18)30135-X ). This study resolves the conflicting data and finally answers the question: “How much carbohydrates should we be eating if we desire a long and healthy life?” The answer is “Enough.”
Such a study has just been published (SB Seidelmann et al, The Lancet, doi.org/10.1016/S2468-2667(18)30135-X ). This study resolves the conflicting data and finally answers the question: “How much carbohydrates should we be eating if we desire a long and healthy life?” The answer is “Enough.”
I call this “The Goldilocks Effect” You may remember “Goldilocks And The Three Bears.” One bed was too hard. One bed was too soft. But, one bed was “just right.” One bowl of porridge was too hot. One was two cold. But, one was “just right.” According to this study, the same is true for carbohydrate intake. High carbohydrate intake is unhealthy. Low carbohydrate intake is unhealthy. But, moderate carbohydrate intake is “just right.”
How Was The Study Done?
This study was performed in two parts. This first part drew on data from the Atherosclerosis Risk in Communities (ARIC) study. That study enrolled 15,428 men and women, aged 45-64, from four US communities between 1987 and 1989. This group was followed for an average of 25 years, during which time 6283 people died. Carbohydrate intake was calculated based on food frequency questionnaires administered when participants enrolled in the study and again 6 years later. The study evaluated the association between carbohydrate intake and mortality.
The second part was a meta-analysis that combined the data from the ARIC study with all major clinical studies since 2007 that measured carbohydrate intake and mortality and lasted 5 years or more. The total number of participants included in this meta-analysis was 432,179, and it included data from both studies that claimed low-carbohydrate intake was associated with decreased mortality.
How Much Carbohydrates Should We Eat?
 The results from the ARIC study were:
The results from the ARIC study were:
- The relationship between mortality and carbohydrate intake was a U-shaped curve.
- The lowest risk of death was observed with a moderate carbohydrate intake (50-55%). This is the intake recommended by current nutrition guidelines.
- The highest risk of death was observed with a low carbohydrate intake (<40%).
- The risk of death also increased with very high carbohydrate intake (>70%).
- When the investigators used the mortality data to estimate life expectancy, they predicted a 50-year old participant would have a projected life expectancy of:
- 1 years if they had a moderate intake of carbohydrates.
- Their life expectancy was 4 years less if they had a low carbohydrate intake.
- Their life expectancy was 1.1 year less if they had a very high carbohydrate intake.
- The risk associated with low carbohydrate intake was affected by what the carbohydrate was replaced with.
- When carbohydrate was replaced with animal protein and animal fat there was an increased risk of mortality on a low-carb diet. The animal-based low-carb diet contained more beef, pork, lamb, chicken and fish. It was also higher in saturated fat.
 When carbohydrate was replaced with plant protein and plant fats, there was a decreased risk of mortality on a low-carb diet. The plant-based low-carb diet contained more nuts, peanut butter, dark or whole grain breads, chocolate, and white bread. It was also higher in polyunsaturated fats.
When carbohydrate was replaced with plant protein and plant fats, there was a decreased risk of mortality on a low-carb diet. The plant-based low-carb diet contained more nuts, peanut butter, dark or whole grain breads, chocolate, and white bread. It was also higher in polyunsaturated fats.- The effect of carbohydrate intake on mortality was virtually the same for all-cause mortality, cardiovascular mortality, and non-cardiovascular mortality.
- There was no significant affect of carbohydrate intake on long-term weight gain (another myth busted).
The results from the meta-analysis were very similar. When the data from all studies were combined:
- Both low carbohydrate diets and very high carbohydrate diets were associated with increased mortality.
- Meat-based low-carb diets increased mortality, and plant-based low-carb diets decreased mortality.
- Once again, the results were the same for total mortality, cardiovascular mortality, and non-cardiovascular mortality.
The authors concluded: “Our findings suggest a negative long-term association between life-expectancy on both low carbohydrate and high carbohydrate diets…These data also provide further evidence that animal-based low carbohydrate diets should be discouraged. Alternatively, when restricting carbohydrate intake, replacement of carbohydrates with predominantly plant-based fats and proteins could be considered as a long-term approach to healthy aging.”
Why Were Some Previous Studies Misleading?
This study also resolved the discrepancies between previous studies. The authors pointed out that the average carbohydrate intake is very different in Europe and the US than in Asian countries and low-income countries. In the US and Europe, mean carbohydrate intake is about 50% of calories and it ranges from 25% to 70% of calories. With that range of carbohydrate intake, it is possible to observe the increase in mortality associated with both low and high carbohydrate intakes.
White rice is a staple in Asian countries, and protein is a garnish rather than a main course. Consequently, overall carbohydrate intake is greater in Asian countries and very few Asians eat a low carbohydrate diet. High protein foods tend to be more expensive than high carbohydrate foods. Thus, very few people in developing countries can afford to follow a low carbohydrate diet, and overall carbohydrate intake also tends to be higher.
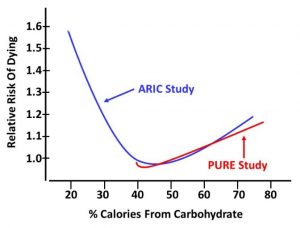 Therefore, in Asian and developing countries the average carbohydrate intake is greater (~61%) than in the US and Europe, and the range of carbohydrate intake is from 45% to 80% of calories. With that range of intake, it is only possible to see the increase in mortality associated with high carbohydrate intake.
Therefore, in Asian and developing countries the average carbohydrate intake is greater (~61%) than in the US and Europe, and the range of carbohydrate intake is from 45% to 80% of calories. With that range of intake, it is only possible to see the increase in mortality associated with high carbohydrate intake.
Both the studies that low-carb enthusiast quote to support their claim that low-carb diets are healthy relied heavily on data from Asian and developing countries. In fact, when the authors of the current study overlaid the data from the PURE study with their ARIC data, there was an almost perfect fit. The only difference was that their ARIC data covered both low and high carbohydrate intake while the PURE study touted by low-carb enthusiasts only covered moderate to high carbohydrate intake. [I have given you my rendition of the graph on the left. If you would like to see the data yourself, look at the paper .]
Basically, low-carb advocates are telling you that diets with carbohydrate intakes of 30% or less are healthy based on studies that did not include carbohydrate intakes below 40%. That is misleading. The studies they quote are incapable of detecting the risks of low carbohydrate diets.
What Does This Mean For You?
There are several important take-home lessons from this study:
- All major studies agree that very high carbohydrate intake is unhealthy. In part, that reflects the fact that diets with high carbohydrate intake are likely to be high in sodas and sugary junk foods. It may also reflect the fact that diets which are high in carbohydrate are inevitably low in protein or healthy fats or both.
 All studies that cover the full range of carbohydrate intake agree that low carbohydrate intake is also unhealthy. It shortens life expectancy of a 50-year old by about 4 years.
All studies that cover the full range of carbohydrate intake agree that low carbohydrate intake is also unhealthy. It shortens life expectancy of a 50-year old by about 4 years.- The studies quoted by low carb enthusiasts to support their claim that low-carb diets are healthy don’t include carbohydrate intakes below 40%. That means their claims are misleading. The studies they quote are incapable of detecting the risks of low carbohydrate diets.
- Meat-based low-carb diets decrease life expectancy while plant-based low carb diets increase life expectancy. This is consistent with previous studies. For more details on those studies, see my article “Are Any Low-Carb Diets Healthy?” in “Health Tips From The Professor” or my book, “Slaying The Food Myths.”
The health risks of meat-based low-carb diets may be due to the saturated fat content or the heavy reliance on red meat. However, the risks are just as likely to be due to the foods these diets leave out – typically fruits, whole grains, legumes, and some vegetables. Proponents of low-carb diets assume that you can make up for the missing nutrients by just taking a multivitamin. However, each food group also provides a unique combination of phytonutrients and fibers. The fibers, in turn, influence your microbiome. Simply put, whenever you leave out whole food groups, you put your health at risk.
Limitations Of This Study
 My main concern with this study and all previous studies is that they lump all carbohydrates together, as if they were equally healthy or unhealthy. We should really be focusing on healthy carbohydrates versus unhealthy carbohydrates, healthy proteins versus unhealthy proteins, and healthy fats versus unhealthy fats. We should be focusing on foods.
My main concern with this study and all previous studies is that they lump all carbohydrates together, as if they were equally healthy or unhealthy. We should really be focusing on healthy carbohydrates versus unhealthy carbohydrates, healthy proteins versus unhealthy proteins, and healthy fats versus unhealthy fats. We should be focusing on foods.
For example, the plant-based low carbohydrate diets in this study probably had a higher percentage of healthy carbohydrates because those diets feature whole, plant-based foods. The very high carbohydrate diets in this study probably had a higher percentage of unhealthy carbohydrates. However, we have no idea whether the diets with moderate carbohydrate intake featured healthy carbohydrates or unhealthy carbohydrates. That is critical because moderate carbohydrate intake was the baseline to which all other diets were compared.
An important unanswered question is: “What is the relationship between carbohydrate intake and lifespan when most of the carbohydrates come from whole, plant-based foods?” Is low carbohydrate intake healthier or less healthy than moderate carbohydrate intake? Is high carbohydrate intake still less healthy? We have no idea. No studies have analyzed the data in that way.
Similarly, we know from multiple studies that meat-based, low-carb diets increase mortality and plant-based, low-carb diets decrease mortality when compared to moderate carbohydrate intake with no differentiation of protein source. But, what if the moderate carbohydrate group had also been subdivided into meat eaters and plant eaters? Would meat-based, low-carb diets still be less healthy than meat-based, moderate-carbohydrate diets? Would plant-based, low-carb diets still be healthier than plant-based, moderate-carb diets? We have no idea.
The Bottom Line
The low-carb wars are raging. Several studies have reported that low-carb diets increase risk of mortality (shorten lifespan). However, two recent studies have come to the opposite conclusion. Those studies have low-carb enthusiasts doing a victory lap and claiming it is time to rewrite nutritional guidelines to favor low-carb diets.
However, a study just published a couple of weeks ago resolves the conflicting data and finally answers the question: “How much carbohydrate should we be eating if we desire a long and healthy life?” The answer is “Enough.”
I call this “The Goldilocks Effect.” According to this study, high carbohydrate intake is unhealthy. Low carbohydrate intake is unhealthy. But, moderate carbohydrate intake is “just right.”
Specifically, this study reported:
- Moderate carbohydrate intake (50-55%) is healthiest. This is also the carbohydrate intake recommended by current nutritional guidelines.
- All major studies agree that very high carbohydrate intake (60-70%) is unhealthy. It shortens life expectancy of a 50-year old by about a year.
- All studies that cover the full range of carbohydrate intake agree that low carbohydrate intake (<40%) is also unhealthy. It shortens life expectancy of a 50-year old by about 4 years.
- The studies quoted by low carb enthusiasts to support their claim that low-carb diets are healthy don’t include carbohydrate intakes below 40%. That means their claims are misleading. The studies they quote are incapable of detecting the risks of low carbohydrate diets.
- Meat-based, low-carb diets decrease life expectancy while plant-based, low carb diets increase life expectancy. This is consistent with the results of previous studies.
The authors concluded: “Our findings suggest a negative long-term association between life-expectancy and both low carbohydrate and high carbohydrate diets…These data also provide further evidence that animal-based low carbohydrate diets should be discouraged. Alternatively, when restricting carbohydrate intake, replacement of carbohydrates with predominantly plant-based fats and proteins could be considered as a long-term approach to healthy aging.”
For more details, read the article above.
These statements have not been evaluated by the Food and Drug Administration. This information is not intended to diagnose, treat, cure or prevent any disease.
